Stay-at-Home Moms: How to Cope With Burnout & Depression?

In this article
People often face burnout, depression, and anxiety when they become parents. However, moms are usually the ones who suffer the most.
Both stay-at-home moms and those experiencing baby blues or postpartum depression may face significant mental health challenges.
Being a stay-at-home mom is hard. In addition to typically bearing the responsibility for many of the family’s daily tasks—like laundry, meal prep, and clean up—stay-at-home moms also often play the central role in managing the family schedule, organizing family activities, taking charge of each person’s to-dos, and holding space for the emotional needs of the household [1] Ciciolla, L., & Luthar, S. S. (2019). Invisible household labor and ramifications for adjustment: Mothers as captains of households. Sex Roles, 81(7–8), 467–486. https://doi.org/10.1007/s11199-018-1001-x .

Moms can also experience depression due to “baby blues.”
Due to hormonal changes, sleep deprivation, and the stress of adjusting to parenthood, 60-80% of new moms experience the “baby blues.” However, around 13%—more than 1 in 8—face a more serious condition: postpartum depression, which is the most common complication of pregnancy.
Being a stay-at-home mom
Being a stay-at-home parent is more common than ever. Stay-at-home parents often juggle multiple roles: caregiver, housekeeper, teacher, chef, accountant, driver, coach.
And it’s hard work. For parents who also work or recently left their careers, workplace depression from gender stress can compound these challenges. It’s also often thought of as invisible work, as it is not rewarded with a paycheck or regarded by mass culture as a high-value position.
Baby blues vs. postpartum depression
After having a baby, many new parents experience an emotional rollercoaster called baby blues. You might feel tired and cranky and have sudden mood swings, going from fine to crying in seconds.
While most moms go through this, it usually starts a few days after birth and fades within two weeks without treatment.

However, if you’re still not bonding with your baby or are overwhelmed with worries about being a bad parent after a couple of weeks, you may be dealing with postpartum depression (PPD).
Postpartum depression symptoms might include:
- You’re often sad, tearful, down, or bummed out
- You have feelings of guilt, inadequacy, or regret (e.g., “I’m not a good mom;” “I shouldn’t have had this child;” “I’m a failure.”)
- You’re not feeling connected or bonded to your baby
- You no longer experience pleasure or joy in things you used to love
- Your eating habits or appetite has changed
- You can’t sleep even when you have the chance to, or you’re sleeping too much
- You’re usually extremely tired and depleted
- You have trouble concentrating and feel slowed down
- You’re afraid of being alone or going outside
- You feel angry, or in a panic, you’re more anxious than usual
- You think about death or suicide or harming your baby
Stay-at-home mom burnout
You’re helping one kid complete her homework assignment when you look across the room and see your younger child coating his feet in the paint for an art project.
Paint on the rug and his clothes, your older child is upset that your attention is split, you’ve had to pee for as long as you can remember, you haven’t eaten since 6 pm the night before, and there is no support in sight.
No wonder stay-at-home mom burnout is so prevalent.
Being a working mom versus a stay-at-home mom has its own set of perks and challenges. Yet, compared to working moms, stay-at-home moms are much more likely to experience physical and mental health issues such as depression, anxiety, and burnout [2] Frech, A., & Damaske, S. (2012). The Relationships between Mothers’ Work Pathways and Physical and Mental Health. Journal of Health and Social Behavior, 53(4), 396–412. https://doi.org/10.1177/0022146512453929 .
Burnout arises from chronic and unremitting stress. The vast majority of research is centered around professional burnout, but it can be translated to being a stay-at-home mom too.
How many people would apply for a job that has no sick leave, no overtime protection, and no pay?
Signs of SAHM burnout and anxiety
If you’re a stay-at-home mom and are feeling drained, disconnected, and inadequate, these are signs that you may be dealing with parental burnout.
Parental burnout is defined as a combination of three distinct experiences [3] Hubert, S., & Aujoulat, I. (2018). Parental burnout: when exhausted mothers open up. Frontiers in Psychology, 9. https://doi.org/10.3389/fpsyg.2018.01021 :
- Feeling physically and emotionally exhausted
- Feeling emotionally distant from your children
- Feeling incompetent as a parent
Stay-at-home mom burnout can also go hand-in-hand with the experience of depression or anxiety. While the vast majority of moms experience the baby blues in the weeks after childbirth, baby blues can also continue into postpartum depression.
Keep an eye out for symptoms such as:
- Fatigue
- Difficulty sleeping
- Irritability
- Tearfulness
- Lack of energy
- Hopelessness
To learn more and explore whether you may be experiencing stay-at-home mom burnout, consider taking this burnout test adapted from the Oldenburg Burnout Inventory.
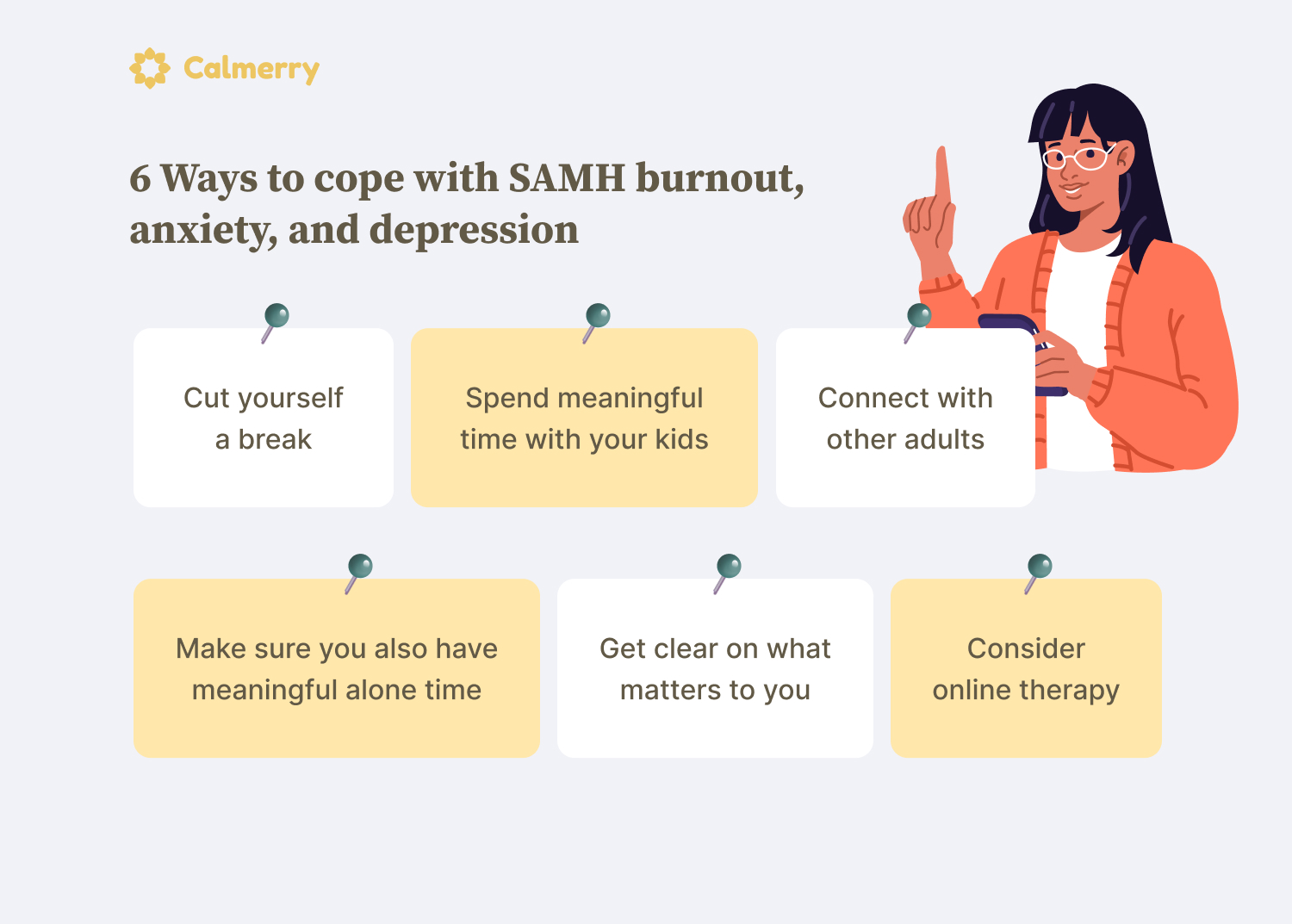
6 Ways to cope with SAHM burnout and depression
The thing with stay-at-home mom burnout is that while you experience this drain on your internal resources, the world keeps spinning, and the demands continue to pile up.
At this point, the question may not even be how to avoid stay-at-home mom burnout but rather what to do about stay-at-home mom burnout.
There are broad, systemic things that would help, like affordable childcare, parental leave, and undoing many of the “isms” that impact stay-at-home moms.
That stuff is not going to change overnight, though, and in the meantime, you still need tools to cope.
As you probably know, managing stay-at-home mom burnout is not simple. It requires more than an occasional act of self-care, like a lavender-infused bath or your favorite takeout.
Those sound lovely, and by all means, partake.
But think of stay-at-home mom burnout as something much larger. Don’t be disappointed to find it still lingering once you throw away the takeout containers or get out of the bath.
Take heart in knowing that it doesn’t have to be this way.
Building resilience and managing mom burnout is a long game. And while the last thing an overstretched mom needs is another to-do, preventing burnout will take some investment. In the end, it’s well worth it.
While avoiding it altogether may not always be in the cards for stay-at-home or working moms, here are 6 strategies to reduce and manage stay-at-home mom burnout, anxiety, and depression.
1. Cut yourself a break
Why is it so easy to be kind and generous to other people but so hard to be that way towards ourselves?
In our culture, women and moms can have very high expectations for themselves. When we feel like we’re not up to par, we tend to be very self-critical with “Everyone else is handling it, why can’t I? What’s wrong with me?”.
When you notice that critical voice in your head, see if you can engage a kinder and wiser voice inside of you. Be gentle with yourself.
There are a lot of opinions on parenting out there, especially if you’re on social media. It can be a wonderful resource and method of connection, but it can also breed loneliness and depression [4] Hunt, M. G., Marx, R., Lipson, C., & Young, J. (2018). No more FOMO: Limiting social media decreases loneliness and depression. Journal of Social and Clinical Psychology, 37(10), 751–768. https://doi.org/10.1521/jscp.2018.37.10.751 .
Know yourself and notice your reactions so you can tune out the noise and tune inward when that is what you most need.
Toys on the floor, a mismatched outfit, and dirty dishes in the sink, while anxiety-provoking, are not going to go down in the history of your life as what is most important.
The truth is, good enough parenting is ideal parenting. You’re creating a model for your children that you do not have to be perfect to be valuable, important, or loved.
2. Spend meaningful time with your kids
This might seem counter-intuitive. Spending too much time with your children is one of the things that cause stay-at-home mom burnout, right?
It turns out that investing in your relationship with your kids and building a connection with them can actually combat burnout.
By engaging in the part of your role as a parent that fills you with purpose, you can find yourself rejuvenated.

To make it as simple as possible, focus on the pieces of parenthood that come most naturally to you and that you enjoy. This could be a walk, sharing a meal, baking, coloring, reading, or learning something new together.
All that matters is that you incorporate consistent time outside of the get-dressed-eat-bathe-bed routine that fills you with meaning and connection.
3. Ensure you have meaningful alone time
As a busy stay-at-home mom, you may feel as though your entire existence is based on supporting others. All mothers had lives before becoming a parent.
Maybe you had a career, a hobby, or something that you dedicated your time and energy to that you no longer do.

By now, you might be thinking, “If I could do that, I wouldn’t be reading this article! But my family lives far away, I can’t afford childcare, my partner works long hours, and I really have no support.”
Your concern is completely valid. Try also to gently push back on the idea that help is absolutely not accessible to you. Think outside the box and see what creative ways you can come up with to get that space.
Perhaps it’s a childcare swap or even a regular quiet time each day at home.
Depending on the ages of your children, this may be when they nap or play in a different room, giving you the time you need for yourself and giving your child a chance to build their creativity, develop their problem-solving skills, and explore their individual identities.
The tricky part is that this is no longer the time to do the dishes or quickly cross off as many to-dos as you can. This is now “you time.” It is the time to do those things that support your identity and fill you with personal meaning.
And it is the time to engage in self-care that is regenerative. If something else doesn’t get done, having this time is still non-negotiable.
4. Connect with other adults
It’s not uncommon to feel lonely and isolated when you’re spending all day with your kids. This can be difficult to talk about as many stay-at-home moms are wracked with guilt trying to live up to impossible expectations.
Yet while solitude can be enriching and vitalizing, loneliness is often draining and painful.
The trouble is, when you’re feeling depressed and burned out, it’s hard to be motivated to reach out to old friends or meet new people. Yet, it is also in our friendships that we often truly connect with ourselves and delight in our connections with others.

Consider reaching out to a friend and making a plan this week. It could be anything: a phone call, a walk, dinner, or a playdate with your kids.
If that sounds like too much, start by going to the park and striking up a conversation with another adult, even for 5 minutes.
If you feel out of practice, remember to go back to the basics. The key ingredients are just to be open, vulnerable, generous, and kind [5] Collins, N. L., & Miller, L. C. (1994). Self-disclosure and liking: A meta-analytic review. Psychological Bulletin, 116(3), 457–475. https://doi.org/10.1037/0033-2909.116.3.457 . And ultimately, you can’t go wrong with being yourself.
5. Get clear on what matters to you
If you take the time to clarify your values, you can then use them as guideposts to help you move through your day. For example, you may value modeling to your children that you have a strong identity outside of being a parent.
Alternatively, you may value centering your children in all of your decisions and offering them steadfast availability and presence.
It’s tempting to compare yourself to your friends, peers, and other parents. But in reality, there’s no right or wrong when it comes to defining your values.
What matters is that when your choices are driven by your honest and authentic values, you gain a sense of confidence, pride, and fulfillment [6] Peterson, C., Ruch, W., Beermann, U., Park, N., & Seligman, M. E. P. (2007). Strengths of character, orientations to happiness, and life satisfaction. The Journal of Positive Psychology, 2(3), 149–156. https://doi.org/10.1080/17439760701228938 .
Living in this way can also strengthen your resilience to the discomforts such as depression and anxiety you face in your day-to-day life as a stay-at-home mom.
6. Consider online therapy
Being a stay-at-home mom can unearth all kinds of deep-seated issues that can be stressful, confusing, and overwhelming. Stay-at-home mom burnout is as real as it gets.
This is not a minor issue to be swept under the rug. On the contrary, it is an actual health problem with real health consequences, including [7] Salvagioni, D. a. J., Melanda, F. N., Mesas, A. E., González, A. D., Gabani, F. L., & De Andrade, S. M. (2017). Physical, psychological and occupational consequences of job burnout: A systematic review of prospective studies. PLoS ONE, 12(10), e0185781. https://doi.org/10.1371/journal.pone.0185781 :
- Diabetes
- Heart disease
- High cholesterol
- Headaches
- Insomnia
- And mental health issues like depression
You’re not supposed to do this all by yourself, nor should you have to. A therapist can help you make sense of your struggles and develop coping strategies and resilience to address stay-at-home mom burnout, depression, and anxiety.
In therapy, you can work together on identifying your values, noticing negative self-talk, figuring out how to ask for help when you need it, and coming up with a plan to support and nourish yourself during this challenging time.
Postpartum depression treatment

As a new parent, PPD affects your health, your experience, and your connection with your baby. In turn, this can impact your baby’s health and lead to eating, sleeping, and behavioral problems later on.
Postpartum depression treatment often includes psychotherapy, sometimes in combination with medications.
Self-care is also an essential piece to managing depression. But when you’re a new parent, it’s not always possible to prioritize sleep, eat healthy foods, and remain active.
Support from your spouse, partner, family members, and friends can go a long way.
Final thoughts
With online therapy for mothers, such as on Calmerry, you can now access high-quality, insightful, and supportive therapists from the comfort of your home. As a busy stay-at-home mom and new parent, you don’t have to find childcare or leave your kids at home alone to get help.
Having a baby is not something you’re going to experience very often in your life, and you don’t have to miss out on it because of depression.
You absolutely deserve the support, and both you and your family will benefit from it!
Ciciolla, L., & Luthar, S. S. (2019). Invisible household labor and ramifications for adjustment: Mothers as captains of households. Sex Roles, 81(7–8), 467–486. https://doi.org/10.1007/s11199-018-1001-x
Frech, A., & Damaske, S. (2012). The Relationships between Mothers’ Work Pathways and Physical and Mental Health. Journal of Health and Social Behavior, 53(4), 396–412. https://doi.org/10.1177/0022146512453929
Hubert, S., & Aujoulat, I. (2018). Parental burnout: when exhausted mothers open up. Frontiers in Psychology, 9. https://doi.org/10.3389/fpsyg.2018.01021
Hunt, M. G., Marx, R., Lipson, C., & Young, J. (2018). No more FOMO: Limiting social media decreases loneliness and depression. Journal of Social and Clinical Psychology, 37(10), 751–768. https://doi.org/10.1521/jscp.2018.37.10.751
Collins, N. L., & Miller, L. C. (1994). Self-disclosure and liking: A meta-analytic review. Psychological Bulletin, 116(3), 457–475. https://doi.org/10.1037/0033-2909.116.3.457
Peterson, C., Ruch, W., Beermann, U., Park, N., & Seligman, M. E. P. (2007). Strengths of character, orientations to happiness, and life satisfaction. The Journal of Positive Psychology, 2(3), 149–156. https://doi.org/10.1080/17439760701228938
Salvagioni, D. a. J., Melanda, F. N., Mesas, A. E., González, A. D., Gabani, F. L., & De Andrade, S. M. (2017). Physical, psychological and occupational consequences of job burnout: A systematic review of prospective studies. PLoS ONE, 12(10), e0185781. https://doi.org/10.1371/journal.pone.0185781
online therapy
live video session




